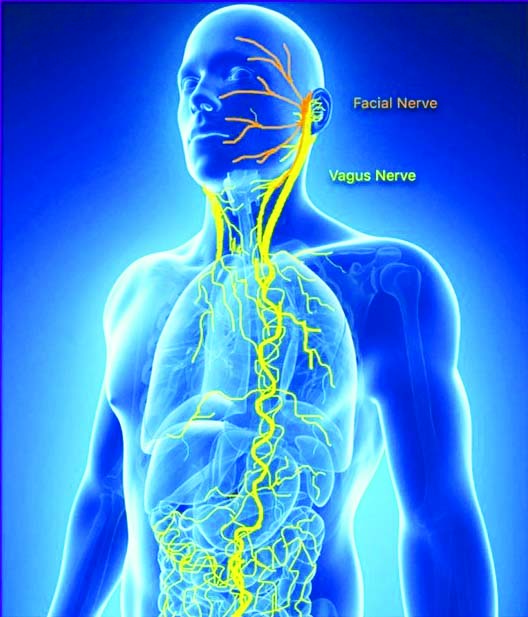
What is the Vagus Nerve?
The vagus nerve is the longest cranial nerve in the body, stretching from the brainstem through the neck and into the chest and abdomen. Its name comes from the Latin word vagus, meaning “wandering” which is fitting given how many organs it touches — including the heart, lungs, and digestive tract.
It’s a core part of the parasympathetic nervous system, which governs the body’s “rest and digest” functions. Unlike the sympathetic nervous system (which controls the “fight, flight, or freeze” stress responses), the parasympathetic system helps the body calm down. Recover, and restore balance.
The vagus nerve is essentially the communication superhighway between the brain and body. It sends signals in both directions, informing the brain about the body’s state and helping regulate vital processes like heart rate, digestion, immune response, and— importantly emotional regulation.
The Vagus Nerve Role in Trauma
When someone experiences trauma— whether from abuse, neglect, violence, or even chronic stress-the nervous system becomes dysregulated. The body may get stuck in a heightened state of alertness, even long after the danger has passed. This is often referred to as a state of hyper vigilance, anxiety, or emotional numbness.
This is where the vagus nerve comes in. Research in the field of neurobiology, particularly by Dr. Stephen Porges (developer of Polyvagal Theory), shows that the vagal tone-how well the vagus functions can deeply influence how a person responds to stress and trauma.
Symptoms of Low Vagal Tone
When the vagus nerve is underactive or dysregulated, it may contribute to many symptoms commonly reported by people with unresolved trauma, such as:
- Chronic anxiety or panic
- Fatigue or low energy
- Difficulty feeling safe in relationships
- Digestive issues (like IBS)
- Sleep disturbances and insomnia
- Feeling disconnected or disassociated
- Depression or mood swings
- Difficulty regulating emotions
- Fatigue or low energy
- Difficulty feeling safe in relationships
These symptoms are not “all in your head” — they are rooted in the nervous system’s ongoing perception of danger and its inability to fully relax or return to a calm state.
Healing Through the Vagus Nerve
The good news is — the vagus nerve can be trained. Just like a muscle, its tone can improve through intentional practices, which can help the nervous system shift from survival mode into a more regulated and resilient state.
Here are a few of the ways to support vagus nerve health and trauma recovery:
Breathwork: Slow, deep diaphragmatic breathing stimulates the vagus nerve and sends calming signals to the brain.
Humming, chanting, or singing. The vagus nerve passed through the throat, so vocal vibration can help stimulate its activity.
Meditation and Mindfulness. These practices build body awareness and help settle the mind and nervous system.
Safe Connection. Engaging in safe, supportive relationships helps rebuild the body’s ability and feel secure with others.
Somatic Therapy and Trauma Informed Coaching ; These modalities work directly with the body’s trauma responses, offering a pathway to healing that goes beyond talk therapy alone.
Why This Matters
Understanding the vagus nerve offers a powerful reframe for people struggling with trauma. It shifts the question from “What’s wrong with me?” to “What happened to my nervous system?” And even more importantly, it opens the door to healing, not by trying to think our way out of trauma, but by learning to regulate and feel safe in our bodies again.
In trauma recovery, safety is the foundation. The vagus nerve plays a vital role in creating that sense of internal safety, and with the right tools and support, healing becomes not just possible-but sustainable.
For an introductory session contact: Sharon Youngblood, Trauma Informed Coach & Somatic Practitioner. E: sharonyoungbood7@gmail.com or call 520-331-1483.